Plantar Fasciitis: Will Physical Therapy Help My Foot Pain?
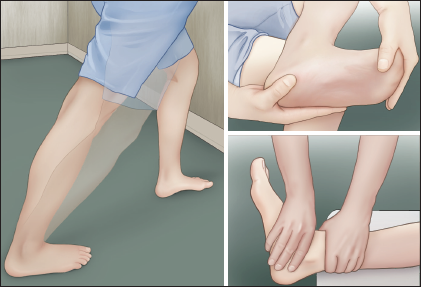
One out of 10 people in the United States experience persistent pain along the bottom of the foot, a condition known as plantar fasciitis. In this country alone, outpatient clinics receive more than 1 million visits a year from people seeking help for this type of foot pain. In 2014, the Orthopaedic Section of the American Physical Therapy Association published updated clinical practice guidelines on the best treatments for patients with plantar fasciitis. The guidelines present evidence that strongly suggests a combination of manual therapy and rehabilitative exercises to help patients with this foot condition. In a more recent study published in the February 2017 issue of JOSPT, researchers reviewed the records of people with plantar fasciitis who were sent to physical therapy to determine whether this treatment lessened their pain.
Anterior Knee Pain: What Muscles Should I Strengthen?
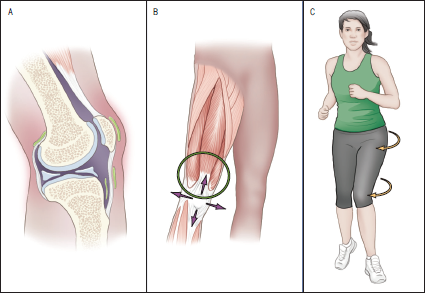
Pain in the front of your knee or under your kneecap is often called patellofemoral pain. You may feel this pain after exercising or when you sit too long. The pain may be a nagging ache or an occasional sharp twinge. Because the pain is around the front of your knee, treatment has traditionally focused on the knee itself and may include taping or bracing the kneecap, or patella, and/or strengthening the thigh muscle—the quadriceps—that helps control your kneecap to improve the contact area between the kneecap and the thigh bone, or femur, beneath it. However, recent evidence suggests that strengthening your hip muscles can also help. The theory is that strong hip muscles can decrease the stress in your knee. A study published in the January 2018 issue of JOSPT provides new insights and evidence-based suggestions on how to strengthen your entire leg to decrease your knee pain and help you return to full activity.
Neck Pain: Clinical Practice Guidelines Help Ensure Quality Care
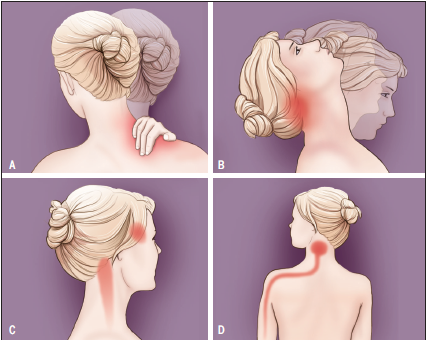
What should patients with neck pain expect from physical therapy? Nine years ago, in 2008, physical therapists published the first neck pain clinical practice guidelines. These guidelines have been updated and are now available in the July 2017 issue of the JOSPT. As before, these guidelines make recommendations based on best practices from scientific research for evaluation, diagnosis, and nonsurgical treatment of neck pain. To update these guidelines, physical therapists teamed with the International Collaboration on Neck Pain to identify leading practices. These revised guidelines provide direction to clinicians as they screen, evaluate, diagnose, and make treatmentbased classifications of neck pain. They also outline the best nonsurgical treatment options based on the published literature. At the end of the day, the best care is a combination of the leading science, the clinical expertise of your health care provider, and your input as the patient. These guidelines help inform the first step in this process.
Running and Osteoarthritis
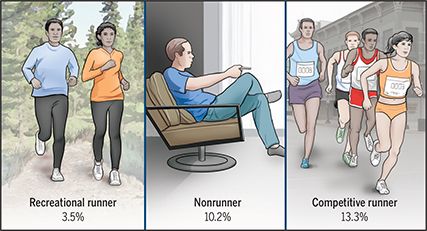
You may have heard the phrase “exercise is medicine.” That’s because exercise, like running, is good for overall health and, specifically, our hearts, lungs, muscles, bones, and brains. Running can also help with weight loss, lower cholesterol levels, boost the immune system, fight depression, reduce stress, and improve mood. No wonder millions of people around the world exercise by running. However, some people are concerned about the impact of running on long- term joint health. Does running lead to higher rates of arthritis in knees and hips? While many researchers find that running protects bone health, others are concerned that this exercise poses a high risk for age-related changes to hips and knees. A study published in the June 2017 issue of JOSPT suggests that the difference in these outcomes depends on the frequency and intensity of running.